搜索结果: 'EasySep Direct'
-
 EasySep™小鼠T细胞分选试剂盒
EasySep™小鼠T细胞分选试剂盒通过免疫磁珠负选获得无磁珠标记的小鼠T细胞
-
 EasySep™小鼠/人嵌合体分选试剂盒
EasySep™小鼠/人嵌合体分选试剂盒对来源于人异种移植受体小鼠的骨髓、脾或外周血样本中未标记人细胞进行免疫磁珠负选分离
-
 EasySep™人FITC正选试剂盒II
EasySep™人FITC正选试剂盒II对来源于外周血单个核细胞或其他单细胞悬液中标记 FITC 缀合抗体的人细胞进行免疫磁珠正选分离
-
 EasySep™人CD14正选试剂盒II 人CD14+细胞的免疫磁珠正选
EasySep™人CD14正选试剂盒II 人CD14+细胞的免疫磁珠正选 -
 EasySep™小鼠CD8+ T细胞分选试剂盒 通过免疫磁珠负选分离无磁珠标记的小鼠CD8+ T细胞
EasySep™小鼠CD8+ T细胞分选试剂盒 通过免疫磁珠负选分离无磁珠标记的小鼠CD8+ T细胞 -
 EasySep™人CD3正选试剂盒II 人CD3+细胞的免疫磁珠正选试剂盒
EasySep™人CD3正选试剂盒II 人CD3+细胞的免疫磁珠正选试剂盒 -
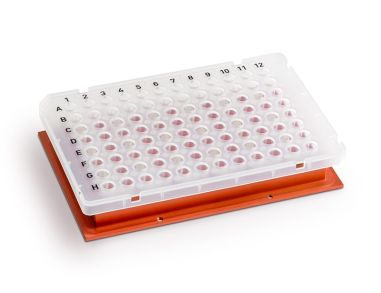 96孔PCR磁力板 无柱核酸提取磁极
96孔PCR磁力板 无柱核酸提取磁极 -
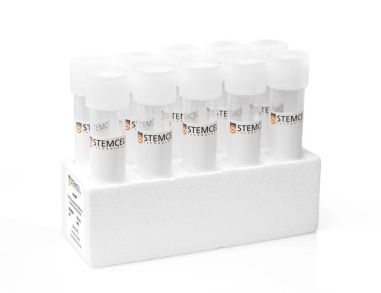 脾脏解离培养基 小鼠脾脏消化解离培养基
脾脏解离培养基 小鼠脾脏消化解离培养基 -
 RoboSep™- S 全自动细胞分选仪器
RoboSep™- S 全自动细胞分选仪器 -
 RoboSep™-16导电滤芯吸头 RoboSep™-16导电滤芯吸头
RoboSep™-16导电滤芯吸头 RoboSep™-16导电滤芯吸头 -
 RoboSep™-16 全自动细胞分选仪器适用于多达16个样本
RoboSep™-16 全自动细胞分选仪器适用于多达16个样本 -
 RoboSep™-16垃圾袋 RoboSep™-16垃圾袋
RoboSep™-16垃圾袋 RoboSep™-16垃圾袋

 EasySep™小鼠TIL(CD45)正选试剂盒
EasySep™小鼠TIL(CD45)正选试剂盒





 沪公网安备31010102008431号
沪公网安备31010102008431号