技术资料
-
 46:01
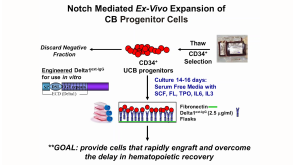
线上讲座Targeting Self-Renewal Function in Normal Hematopoietic and Leukemic Stem Cells发布日期: 02/03/2017
46:01
线上讲座Targeting Self-Renewal Function in Normal Hematopoietic and Leukemic Stem Cells发布日期: 02/03/2017

 EasySep™小鼠TIL(CD45)正选试剂盒
EasySep™小鼠TIL(CD45)正选试剂盒





 沪公网安备31010102008431号
沪公网安备31010102008431号