技术资料
-
 科学海报A Feeder-Free and Serum-Free Culture System Supports Expansion of CD34+ AML and CML Stem/Progenitor Cells
科学海报A Feeder-Free and Serum-Free Culture System Supports Expansion of CD34+ AML and CML Stem/Progenitor CellsConference:
ISEH 2019
-
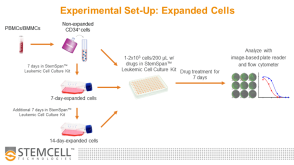
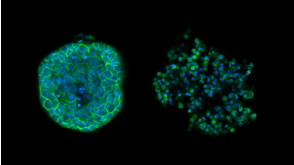
 科学海报Drug Screening and Phenotypic Analysis in a Microwell-based 3D Cell Culture System
科学海报Drug Screening and Phenotypic Analysis in a Microwell-based 3D Cell Culture SystemConference:
AACR 2018

 EasySep™小鼠TIL(CD45)正选试剂盒
EasySep™小鼠TIL(CD45)正选试剂盒













 沪公网安备31010102008431号
沪公网安备31010102008431号